At 39+5, my water broke at 3.30pm just as I woke up from a nice afternoon nap. Although I had been waiting for signs of labor, my initial reaction was confusion. What are we supposed to do now? During all the birth preparation classes, the educators had talked about how in the movies pregnant women always have their water break in public, and that’s how their labor starts, but in reality less than 10% of labors begin in this way. So I had put this scenario out of my mind, since it clearly wasn’t going to happen to me. And so, when it did, I didn’t have a plan. We just weren’t prepared for this.

Last ‘pregnancy picture’. We took this right after my water broke.
I knew that once the water breaks, a 24-hour rule takes effect when you’re delivering at a hospital. Since the water breaking means that there is now an opening from the outside world to the baby’s otherwise sterile environment, this event increases the risk of the baby getting an infection. For that reason, many practitioners have the policy of wanting the baby to be out, or labor to be relatively far advanced, by the 24-hour mark after the water has broken.
So the clock was ticking right away. We called the midwives at the hospital and informed them of the situation. They suggested we come in so they could check me and determine if my water had in fact broken (I knew it had, I don’t think you could really mistake that feeling if you were simply peeing a little bit). But they were also quite calm about the situation, and let us decide when we wanted to come in. We then called Christina, our doula, which I now wish we had done first. You see, we had planned to labor at home until active labor was well established, and going to the hospital would likely derail this (we didn’t know at this point that it definitely would). But because I hadn’t considered this scenario as a possibility for my labor, I defaulted to policy rather than the ‘stop and think about it’ approach we had adopted together with our doula. It turns out that many women don’t inform the hospital of their water breaking right away, exactly so that they can approach labor as they envision, without being limited by a somewhat arbitrary timeline.
Anyway, we let Christina know that we had agreed to get to the hospital within the next couple of hours. We arranged that she would meet us there, so she would be there when they triaged me. Then I persuaded my mom that we really needed to finish baking the Christmas cookies now, before we wouldn’t have time anymore. Of course, this ended with her doing all the baking herself, as I became increasingly focused on the workings of my body. I was anxious to get labor started with proper contractions, of which I had had absolutely none at this point. Pain-free, no longer inhibited by the end of pregnancy need to ‘take it easy’, and probably somewhat amped up on adrenaline, I persuaded Paulus out on a nice, brisk walk. During which I climbed every staircase and walked one leg up, the other down on every road + curb constellation I encountered, in an attempt to encourage the baby to move down into the pelvis. When we came home, I noticed that the fluid I was leaking had turned bloody. For some reason, I didn’t think that the blood was supposed to be as bright as it was, and I got worried that something was wrong. So we called the hospital again and let them know we were on our way.
By 5.30pm, we were admitted to what seemed like a completely empty triage ward. Paulus, my mom, and I were let into a triage room, where we waited for a midwife to come examine me. Paulus and I had brought our hospital bags etc., just in case, but for the moment we still didn’t know if they would send us home, allow us to go home, or admit us for real. While we were waiting, Christina joined us. She reminded us that we always had the option of asking for time to consider what the nurses and midwifes proposed, and that if we still wanted to labor at home, we should make sure to ask not to be admitted. After a short wait, the midwife showed up. This was not someone we had seen before, but she was calm and reassuring. She examined me, and found that my water had indeed broken. And then she told us that we would not be allowed to go home. Or, that is, we could go home, but then we wouldn’t be admitted to the birth center anymore, we would have to go to the regular labor and delivery. It was a strange situation, in which we could tell that the midwife herself would have been happy to let us leave to go labor at home, but hospital policy did not allow it. So we decided to stay put. Although it wasn’t what we had planned, I wasn’t particularly disappointed about this, because I knew that the birth center rooms were nice, and I had faith that we would be left alone to labor as much as possible.

Our room in the birth center. We brought all the snacks, including the cookies I had made my mom bake when I realized we would have to go to the hospital…

Checking the baby’s heartbeat with the doppler. Every two hours…
And so we treated our first night in the hospital as a hotel stay. Christina went to drive my mom back to where she was staying, and to pick us up some take-away food. I still wasn’t having any contractions, so we didn’t expect anything to happen until the next morning at the earliest. After Paulus and I unpacked a little, I took a nice warm shower. While in the shower, I started to feel some weak contractions, similar to mild menstrual cramps. They picked up a little as we consumed our dinner, but they were still decidedly mild. Afterwards, we decided to go to bed to get some rest.
In keeping with our hotel theme, we tried to make the atmosphere romantic. We turned the lights off, put on the fake fireplace on the tv, and a nurse brought us some (electric) candles. Then we snuggled up in the double bed to enjoy what might be our last night as a family of two. And if any kissing and such were to have happened, this would serve the dual function of increasing the romance and increasing my oxytocin levels and advancing labor.

The view from the hospital
Another doppler check. The baby is still going strong.
It wasn’t long before my contractions picked up. During the first half of the night, I was able to deal with them myself, by breathing deeply. They still weren’t exactly painful, but they were strong enough that I couldn’t sleep through them, and thus didn’t really get any rest. At some point, Paulus got involved, but most of the night passed in a sort of blur. My contractions were coming more regularly, and they were getting longer.
By early morning, I was really feeling it. When we timed the contractions, they were 2-3 minutes apart and lasted around 50-60 seconds. I could no longer lay down during contractions, and we decided to call Christina and ask her to join us. Room service stopped by, and we ordered breakfast, but at this point (and for the next many hours) I didn’t feel like eating at all, and everything I made myself eat felt like dust in my mouth. Increasingly, I needed to turn my focus inwards during the surges.

Resting in between contractions.
I honestly don’t remember much of what happened during this day. I didn’t have much concept of time, except that every hour or so, a nurse came to take my vitals and listen to the baby with the Doppler. I know that I moved around the room a lot – I leaned over counters, sat on the birthing ball, leaned on the ball, stood/hung with my arms around Paulus’ neck. I needed to be able to move my hips, so I favored the positions that allowed this. At some point Christina suggested that we take a walk around the hospital ward. I agreed to this, but we only made it to the visitor’s room, which was about 20 steps away. Then I leaned over some counters there, before I declared that I wanted to go back. I guess we ordered lunch at some point, but I don’t remember neither what or when. I remember we did some rebozo exercises at some point during the day, and that they helped relieve some of the tension that stayed with me between contractions. I also threw up at some point.

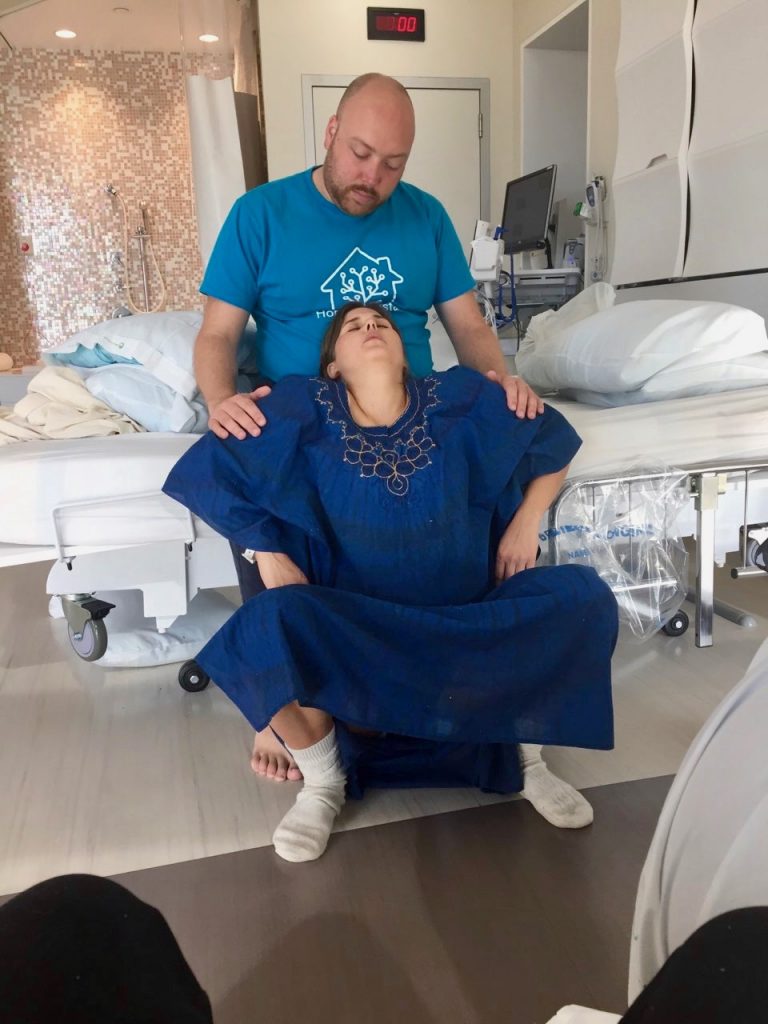
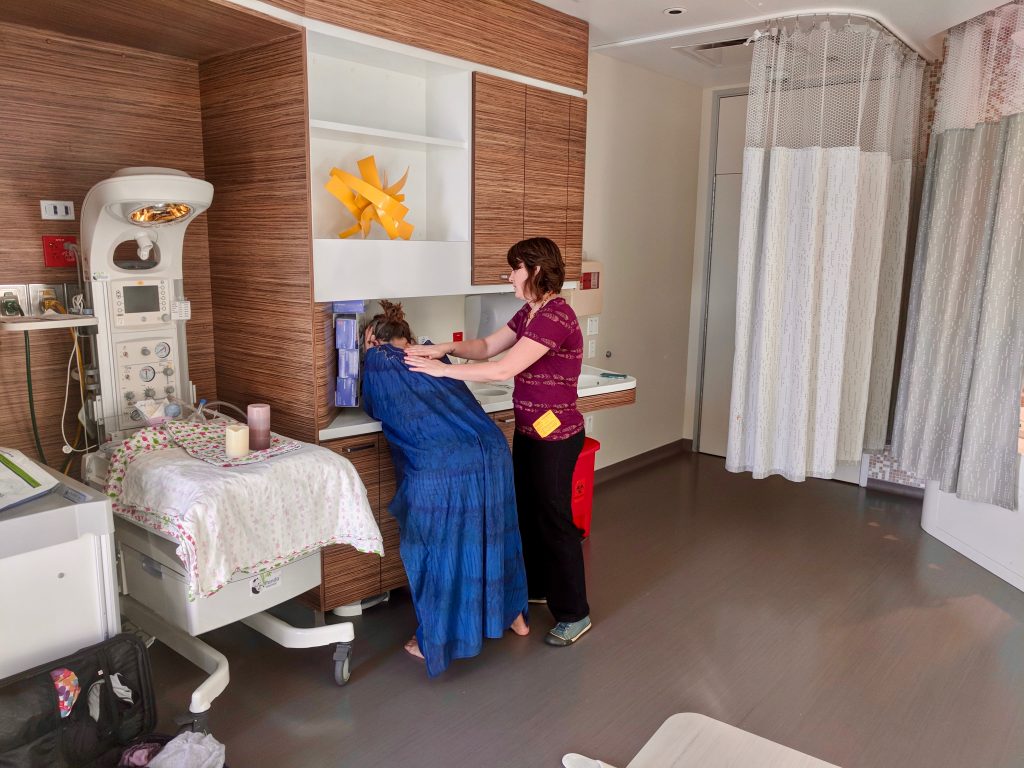
Suddenly, I started feeling strange. There was a lot of pressure in and around my abdomen, and I thought this might be what they refer to as the urge to push. It mostly felt like my pelvic region was trying to flip inside out. My progress (dilation and effacement) hadn’t been checked at this point, so for all I knew, I could be fully dilated. As we were coming up on the 24 hour mark of my water breaking, we decided to ask the midwife to do a check. To some disappointment, the midwife told us that I had only dilated about 3 centimeters at this point. So, clearly not ready to push… My cervix was fully effaced, though, so I took comfort in the fact that I had clearly made some progress. And best of all, the midwife who checked me decided that although I had not quite reached the dilation of 4 cm or more which is usually required to be considered in active labor, my contractions were strong enough and close enough together that they would let me stay to labor in the birth center. So we did.
Again, the next many hours passed in a blur of contraction after contraction. For some reason, I never felt right about using the breathing techniques that I had been practicing so religiously for week leading up to the birth. I gave them a try during a couple of contractions, but it never felt right. Instead, I tried to breathe slowly and vocalize in a low voice register, as suggested by Ina May Gaskin’s book (one of the many birth prep books I had been reading). Paulus and Christina alternated in providing counter-pressure or hands-on comfort during my contractions. These became more painful and got somewhat longer (although I think it was very few of them that ever lasted beyond a minute). And I was getting exhausted. I knew from our birth preparation classes that the most common reason why laboring women request medical pain relief is not actually pain, but exhaustion. I knew this even as I was feeling it, but being it in, there was little I could do. I tried to rest, but with contractions coming minutes apart and me not being able to stand lying down when they occurred, this became increasingly difficult. And although I was able to make myself drink water, eating continued to be an unpleasant chore that I mostly avoided.
A seemingly never ending period of time followed where I would rest on the bed for a minute, then feel a contraction coming on and frantically reach out to Paulus to come pull me up from the bed again. Then I would hang my arms around his neck and we would sway together as I moaned through the contraction, and he whispered encouragements to me. Then the contraction would subside, and I would manage an ‘okay’ to signal Paulus to bring me back to the bed. I don’t know how long this lasted, but it felt like forever, mostly because the contractions continued to feel like they were wringing me inside out, like things were going to fall out of me. And so I began anticipating the contractions with a lot of anxiety and it became increasingly harder to relax as they were happening. I’ll never know if this fear and inability to let go of my tension was related to what happened next, but it is possible. Around 9 pm, I was checked again, and my midwife gave me the bad news that I had not progressed at all since the last check – my dilation was still at 3 cm. At this point, we had long exceeded the 24-hour limit, and with no progress, this was the end of my stay in the birth center. No matter how we chose to proceed, I would be transferred to the regular labor and delivery ward. My midwife, who happened to be the one I had seen most frequently in the clinic, and in whose approach I had a lot of faith and trust, urged me to augment my labor with pitocin. We asked for and were given time to discuss our options, me, Paulus and our doula. We decided to go with the pitocin. Christina and my midwife were both confident that I could manage pitocin-induced labor without pain medication, but I was not. I tried to let their confidence persuade me, but the very thought of trying to relax through magnified contractions while constrained to the bed (as pitocin is given through an IV drip) made my insides knot all up. And as I still had so far to go before full dilation, I was likely looking at another sleepless night. I couldn’t face it. So I asked for information about having epidural anesthesia, and in the end I decided to go with that. Paulus agreed with my choice. Although we had wanted an unmedicated labor, I found that I was ok with changing the plan, given how many unanticipated events had occurred.
It still took a number of hours before we were transferred to the labor and delivery ward and set up in the new room. It was past midnight by the time I got the epidural. During those hours, my contractions slowed down, until they were more than five minutes apart. Perhaps this was a mind-to-body effect of my realizing that I wasn’t going to have an unmedicated labor, but I took it as a sign that I had made the right decision in how I had chosen to proceed with augmentation, etc.
I was hooked up to monitors and beepers and stuff until it felt like I had tubes and wires from all parts of my body. What a stark contrast this presented to our time in the birth center. I felt very happy that I had had the birth center experience, because it enabled me to remain distanced from the medical treatment of birth, and not allow it to define my experience. I still believe that birth is not a medical event, and I hope that if I’m ever pregnant again, that I’ll get to go unmedicated all the way. But I also suspect that I will have to choose care that is not hospital based to ensure that this will happen.
Once everything was set up, we all settled down to get some much needed rest. I fell into an exhausted sleep and didn’t wake until some time past 7am the next morning. A new midwife came to see me, and I was happy to see that this was the very first midwife I had seen at the clinic during my pregnancy, a person who I had liked very much. She checked on my progress, and it was with a sigh of relief that I absorbed the news that I had dilated to six centimeters in the course of the night. So we decided I would be checked again around noon, and hopefully I would have progressed even further then.
So we had breakfast (and I was able to eat something, yay!), then called my mom to let her know all was ok and that she should come to the hospital after lunch. And then we waited. I was still numb from the epidural, but Christina and the nurses helped me get my legs into a butterfly position and later onto a peanut ball, all to help my pelvis widen and encourage the baby to move down. Then we waited. I felt calm and very in-the-moment. Possibly because things were finally moving forward and it was now clear that we would get to meet our baby this day. And possibly this was also an effect of the anesthesia. In any case, Paulus was the complete opposite of me, restless and impatient. But we waited nonetheless.

Stanley Shark with the breastfeeding pillow. Waiting to meet their new friend.
Doing pelvis opening exercises while waiting.
I had discussed the pushing phase with Christina. I really wanted to do the pushing as un-coached as possible, and she suggested that it would be helpful for me to feel the contractions, which might be achieved by reducing the strength of the epidural. We bought this up with the midwife and nurses, and although they were a little bit skeptical about it at first, they agreed once the anesthesiologist had given her ok. So the plan was to reduce the strength of the epidural once I was fully dilated, and then for me to ‘labor down’. Laboring down was a new concept for me, perhaps again because I had not planned on having a medicated delivery (although laboring down is not restricted to those circumstances). Anyway, it’s a pretty neat concept. It just involved waiting. Waiting, instead of immediately pushing, once you’re fully dilated, and thus letting the body and the baby do their own thing. What happens is that the work of the uterus and the baby lets the baby move down the birth canal. That means that you conserve energy for the last bit of pushing, and it is also supposed to reduce tearing of the tissues, I guess because it is less forceful. Anyway, by not going immediately into pushing, we would at the same time allow for laboring down, and for the epidural to wear off a bit.
Noon arrived, and so did my mom. Some time after this, I was checked again. I was finally fully dilated. And thus began more waiting. At 2pm, the midwife and nurse began getting things ready for the delivery. And then it was time to go. Although at this point, I was able to feel my contractions, I never experienced an urge to push, which I was a little sad about. But it was time to do it, nevertheless. So with the help of Paulus and Christina to hold my legs (the epidural had not weakened enough for me to fully control my legs yet), I began actively pushing the baby out. It took a trial push for me to get the hang of it, to figure out which of the muscles that I was barely feeling to activate. I took a deep breath, held it, and pushed as hard as I could. Almost immediately, the baby’s head was crowning. I was able to follow along in the mirror that we had asked to be placed in front of me. In there, I could see a tiny, wrinkled baby scalp emerging, with thick dark hair. The midwife encouraged me to reach down and touch the head, which I did. How surreal and amazing to be touching my baby before he was actually born. To feel him from the outside while he was transitioning from womb-creature to actual person.
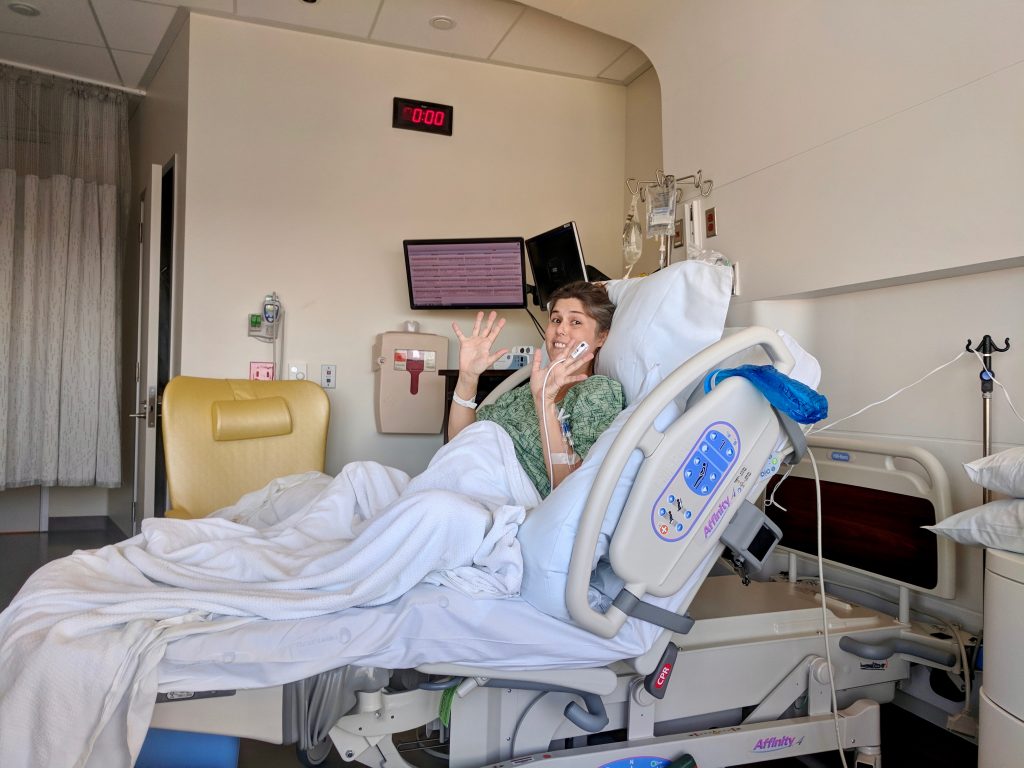
10 cm dilated and clearly excited about it.
Once I really had the hang of the pushing, my midwife let me know that she would quickly go and check on another labor that she was attending. I continued pushing, but after a short while the nurse told me that I had to stop pushing, and breathe during the contractions instead, as the baby was now emerging so quickly, that she would have to call back the midwife, lest the baby be born without her. So my midwife returned, and then there was lots of activity for a moment, and lots of plastic being set up. I don’t remember much of it, only that I hadn’t thought about how hospitals avoid having all the blood and fluids spill on the floor. And that I was anxious to get rid of the hospital gown so that I would meet the baby skin-to-skin.
And then it was go time. A few more pushes brought out the baby’s head. Paulus, who we had wanted to catch the baby, now got to put his hands on the baby’s head, under the midwife’s, as they assisted the baby in turning to allow the shoulders to emerge. Then they emerged – so fast- and Paulus was putting the baby on my chest, letting me know that our baby was a boy. And there he was, such an amazing little creature. I just held him and gazed at him, and then I cried a little, whispering hello to the baby over and over. I helped the nurse rub him down, and Paulus and I had a brief moment with each other, just to look at each other and kiss, and marvel at what we had created together.
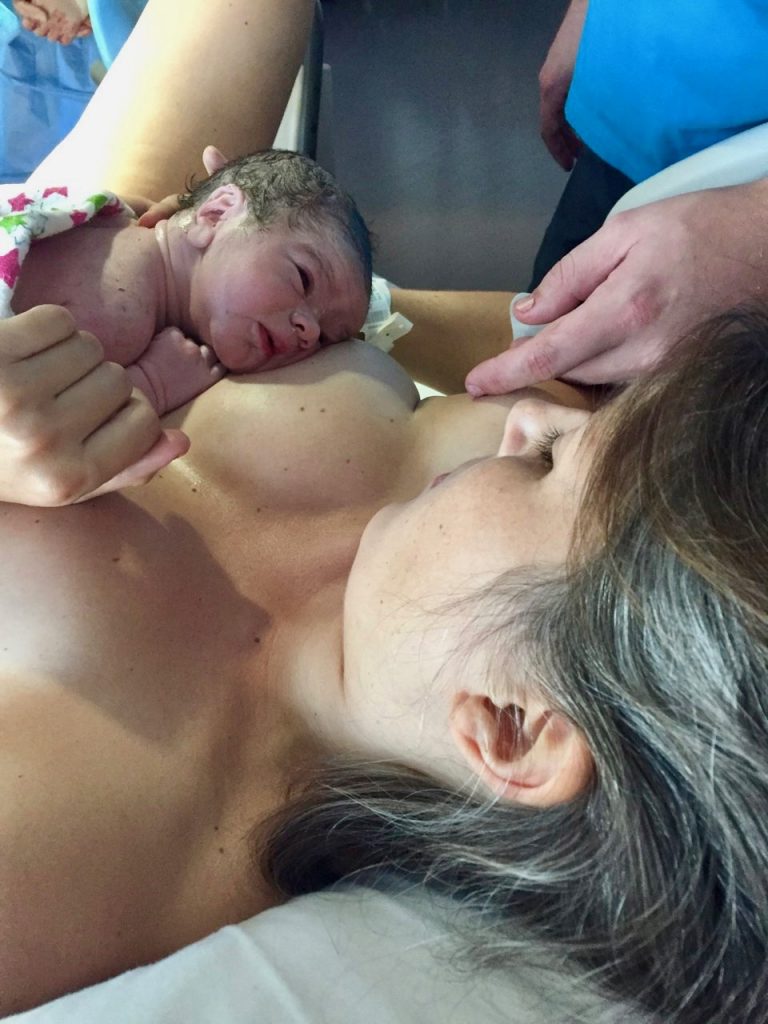

Lots of activity was happening at the other end of the bed (at some point I was asked to push to birth the placenta, and I also had some stitches..), but I realized very little of it. Before long, the baby was looking for the breast, and I focused on helping him latch on. I’m not sure what happened next, but there were lots of baby snuggles, and we got my mom back in the room to meet her grandson, and he was weighed and measured and swaddled. And then we were a family of three.
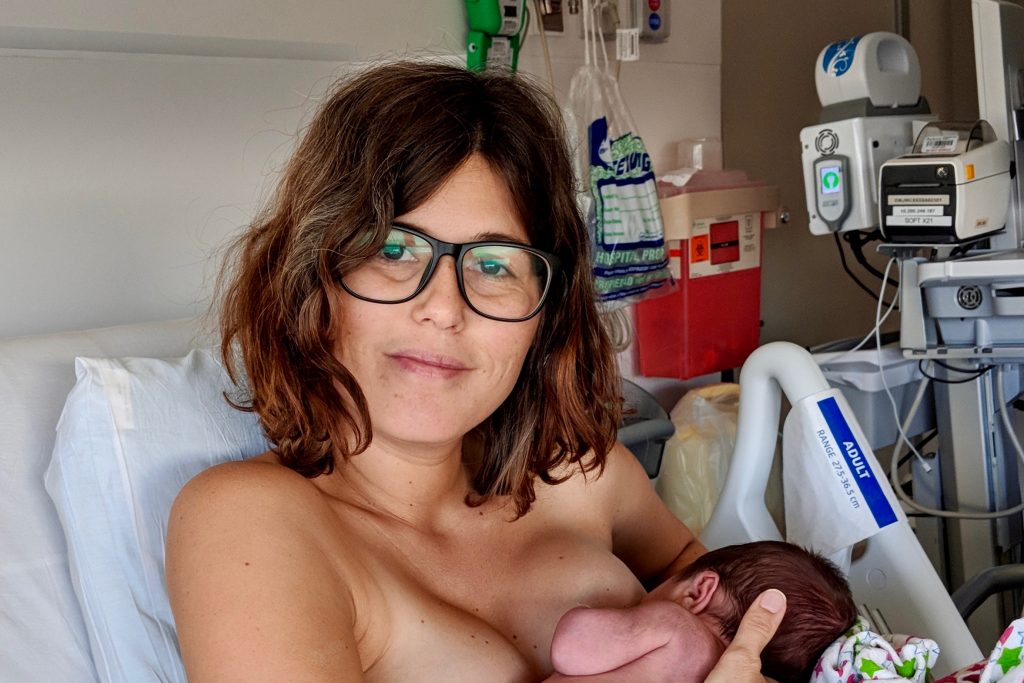
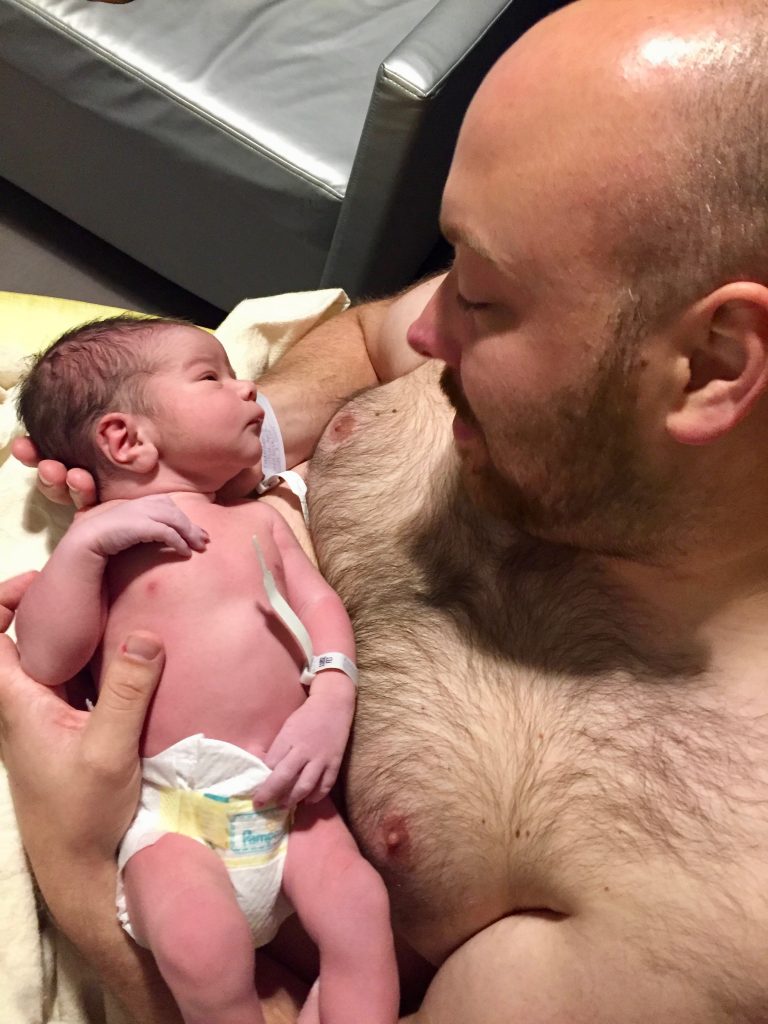

In the evening, still in the hospital (and me still in the bed), we had a big dinner to celebrate. And Paulus changed his first diaper, and there were many more snuggles. And we made it official that we would name our baby Storm. Finally, he is here.





Theo says
a beautiful ending to the story that started 9 months earlier. Enjoy Storm and your little family
Loves
Gitte Frederiksen says
I actually already had forgotten most of this, but you did so well , both of you.
Thank you for letting me be a part of this.😍
Rima says
It really is incredibly emotional ….congrats
Jessica Hilt says
Fantastic birth story! I can’t wait to meet him! I never felt the urge to push either. My birth was unmedicated so it may not have been the epidural. I kept waiting for it. Excellent job, Mama! You did so great. Welcome to the club!